Springer International Publishing Switzerland 2016
Porcia B. Love and Roopal V. Kundu (eds.) Clinical Cases in Skin of Color Clinical Cases in Dermatology 10.1007/978-3-319-22392-6_1
1. Acne Vulgaris
Keywords
Acne vulgaris Benzoyl peroxide/clindamycin gel Tretinoin Doxycycline Propionobacter acnes Postinflammatory hyperpigmentation Keloids Retinoids Clindamycin Erythromycin Doxycycline Azelaic acid Hydroquinone Exogenous ochronosis Minocycline Trimethoprim-sulfamethoxazole Cephalosporins Isotretinoin Oral contraceptives Spironolactone Chemical peels Salicylic acid peels Sunscreen Pomade acne
Case Presentation
A 30-year old African American female presented with a 2-year history of intermittent bumps on her face. She had previously tried numerous over the counter treatments, including topical benzoyl peroxide foams and salicylic acid cleansers. She also used shea butter on her face to help even out her skin tone. Her menstrual cycles were normal.
Physical Examination
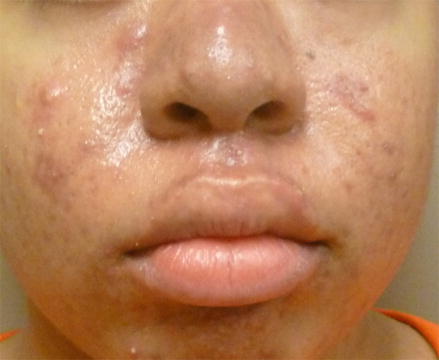
On examination, multiple erythematous papules and pustules and enlarged pores were noted on the cheeks, nose, jawline, and chin. Hyperpigmented macules were also noted on the cheeks and the jawline. A 1 cm erythematous cyst was noted on the right nasal sidewall (Fig. ). Hyperpigmented macules and papules were noted on the chest and upper back.
Figure 1.1
Inflammatory acne vulgaris. Multiple erythematous papules and pustules and enlarged pores are noted on the cheeks, nose, jawline, and chin. Hyperpigmented macules are also noted on the cheeks and the jawline. An erythematous cyst is noted on the right nasal sidewall
Differential Diagnosis
Comedonal acne should be distinguished from acneiform eruptions from follicular occlusion, like pomade and occupational acne. Sebaceous hyperplasia, characterized by yellowish, indurated papules on the forehead and cheeks, is common in adults. Inflammatory acne can be confused with folliculitis (staphylococcal, gram negative, or eosinophilic). Lesions from folliculitis are typically monomorphic papules, and comedones are not present. Papulopustular rosacea favors the forehead, malar region, and the chin. Patients also have telangiectasias and report a history of flushing. Although rosacea typically occurs at a later age, both acne and rosacea can occur in a single individual. Perioral dermatitis is characterized by monomorphic papules and pustules, usually resulting from prolonged use of corticosteroids. Neurotic excoriations on the face, chest, and back can also be confused with acne (Zaenglein and Thiboutot ).
Histopathology
Acne is a clinical diagnosis, and biopsy is typically not indicated. However, biopsy of an acneiform lesion shows a microcomedo with infundibular dilatation and narrowing of the follicular opening. As the follicular epithelium distends, cystic contents rupture into the dermis. The acute inflammatory reaction is characterized by neutrophils creating pustules, foreign body granulation tissue, and subsequent end stage scarring (Zaenglein and Thiboutot ).
Case Treatment
A gentle cleanser was recommended for both morning and evening. A combination benzoyl peroxide/clindamycin gel was recommended for the morning, and a tretinoin 0.1 % cream was recommended for the evening. The patient was also started on doxycycline 100 mg twice daily. A moisturizer with a broad spectrum sunscreen (SPF 30) was recommended for the morning. This same moisturizer was recommended for the evening to prevent irritation from tretinoin. She was advised to discontinue her use of shea butter, as it is typically comedogenic. She was seen back in clinic in 3 months to attempt to taper the doxycycline.
Discussion
Acne is one of the most common skin disorders in people with skin of color. Practice surveys at the Skin of Color Center in New York City (Alexis et al. ) reported that acne vulgaris was the most common diagnosis in patients with skin of color, accounting for 28 % of dermatoses.
The pathogenesis of acne is due to four well known factors: excessive sebum production; abnormal follicular keratinization and plugging; proliferation of Propionobacter acnes ; Hormone changes also contribute to acne pathogenesis. (Callender ).
Clinically, acne vulgaris is characterized by open and closed comedones, papules, pustules, nodules, and cysts (Fig. ).
Figure 1.2
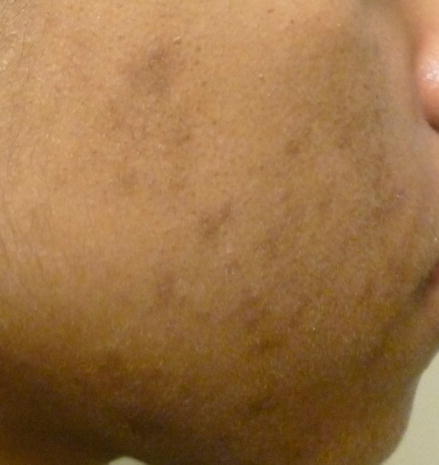
Postinflammatory hyperpigmentation secondary to acne. Hyperpigmented macules are noted on the forehead, cheeks, and jawline
Although acne treatment for patients with skin of color are similar to those for patients with lighter skin, specific considerations exist, especially due to the risk of PIH. Clinically, PIH presents as hyperpigmented macules or patches which correspond to the area of injury. Postinflammatory hyperpigmentation can develop in response to the acne itself or to any overly aggressive acne treatment that disturbs the skin. Postinflammatory hyperpigmentation is thought to be a default pathophysiologic response of darker skin to cutaneous injury in which the inflammation triggers an increase in epidermal or dermal melanogenesis from labile melanocytes (Callender ). For many patients, the lingering PIH is more psychologically disturbing than the acne itself.
Permanent and disfiguring keloid formation is also more common following acne in skin of color. The biologic basis for a tendency for scarring in patients with skin of color may involve differences in fibroblast size and activity, immune related cellular actions, and growth factorsall of which seem to combine to promote production of excess collagen and inhibit degradation of the extracellular matrix (Callender ).
Hair care practices among patients with skin of color may also cause a unique form of acne known as pomade acne. The daily use of pomades on the hair and scalp to overcome an inherent tendency for hair dryness and fragility often leads to a characteristic distribution of comedonal acne on the forehead and anterior hair line (Callender ).
Treatment
The treatment of acne in patients with skin of color can present unique challenges, both pathophysiologically (i.e., risk of PIH and keloid scarring) and culturally (i.e., use of skin and hair care products). The overall goal of acne management is to select treatment that addresses as many of its pathogenic factors as possible while minimizing potential PIH (Alexis et al. ). Because acne treatment can cause cutaneous irritation that initiates or exacerbates PIH in darker-skinned patients, the patients skin should be carefully assessed to determine the risk of irritant contact dermatitis.
Topical retinoids are the top choice for first line therapy, as not only do they target hyperkeratinization and comedogenesis, but they also possess direct anti-inflammatory and antifibroblastic actions, and may block the key pathophysiologic pathways leading to PIH and keloids (Callender ).